Systemic Lupus Erythematosus (Lupus: Gr. Fox) is a complex autoimmune disease with debilitating ill health. Usually, it manifests with heterogeneous features and relapses and remissions involving multiple organ systems. The involvement of kidneys, blood vessels, and the nervous system can be life-threatening. The prevalence of SLE in India is estimated to be 30 per million people. Females are affected more frequently (10:1) than males. SLE is a frequently overlooked disease due to a lack of awareness. The average diagnostic delay is almost four years. On the other hand, SLE is often overdiagnosed based on positive laboratory results in the absence of appropriate clinical features.
Causes
Failure to maintain self-tolerance due to defective immune regulation is the primary defect in SLE. Apoptosis (programmed cell death) of senescent cells brings intracellular molecules to the cell surface. These act as self-antigens and induce tolerance. A wide variety of autoantibodies are generated against these antigens. These autoantibodies damage various tissues directly or indirectly.
SLE is a puzzle. Genetic factors (clustering in families), female sex, hormones, drugs (e.g., minocycline), and environmental factors (sunlight, silica, mercury, Epstein Barr, and other viruses) are important in the development of SLE.
Symptoms
Various clinical features of SLE are enlisted below:
- Fever, generalized pain, fatigue, hair loss, weakness, weight loss
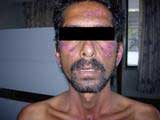
- Butterfly rash on face, various types of rashes in other areas, bleeding under skin, swelling
- Joint pain, swelling, deformities
- Bone pains, fractures, Vitamin D deficiency
- Abdominal pain, bowel perforation, fluid in the abdomen, difficulty in swallowing, liver enlargement
- Breathlessness, fluid around lungs, pneumonia
- Fluid around heart, heart valve abnormalities
- Blood in urine, protein loss from kidneys
- Headache, convulsions, confusion, abnormal movements, neuropathy
- Anxiety, psychosis, mood disorders, cognitive dysfunction
Investigations
Various blood tests, X-rays, and other investigations are performed to evaluate systemic involvement in SLE. Antinuclear antibodies in the blood are tested for diagnosis, prediction of future course, and follow-up of SLE patients. Immunofluorescence with Hep2 cells substrate is currently the most accepted method of ANA determination. ANA can be positive, usually low titer in up to 15 % of normal healthy adults. ANA positivity must, therefore, be interpreted along with clinical features in a given patient. Immunoblotting for analysis of extra-nuclear antigen and estimation of anti-dsDNA antibodies are further tests required in ANA-positive patients.
Assessment
Rheumatologists are trained to assess individual patients with various disease activity and damage indices. Such assessment is essential in planning therapy and knowing the response to treatment. Therapy can be altered according to the adequacy of response.
Treatment
The goals of SLE therapy include rapid induction of remission, prevention of flares, and treatment of comorbidities such as drug effects, diabetes, blood pressure, and vascular disease. Steroid drugs are a cornerstone in the management of SLE. They can be used in varying doses according to disease severity. Hydroxychloroquine, azathioprine, methotrexate, cyclophosphamide, and mycophenolate are important drugs in management. In addition, newer biological agents such as rituximab can be used in nonresponsive patients. Exercise, maintenance of appropriate body weight, proper diet, low dose aspirin, statins for hyperlipidemia, calcium, vitamin D, and avoidance of exposure to sunlight are also essential components of management.
Prognosis
The prognosis in SLE has considerably improved in recent years due to aggressive management strategies. Currently, over 80 % of patients survive up to 15 years. The risk of cancer and involvement of kidneys or nervous system are the major factors deciding prognosis.
Kidney disease in SLE
70 % of patients with SLE have kidney involvement. The risk of progression to end-stage renal disease is up to 25 %. Kidney disease must, therefore, be adequately diagnosed at the earliest stage and aggressively treated. Delay in diagnosis and inadequate therapy lead to treatment failures. 25 % of cases with kidney disease may not respond to treatment and can require kidney transplantation. The graft survival rate in these patients is similar to the general population. However, there is a small chance of recurrence of nephritis after transplantation.
Pregnancy and SLE
Pregnancy is an acceptable risk in SLE patients. Pregnancy should be planned when the disease is quiescent. Mild lupus flare related to the skin can occur in some cases during late pregnancy or after delivery. Hypertension, preterm delivery, pregnancy loss, and fetal morbidity are known complications of pregnancy in SLE. However, pregnancy outcome in SLE patients has significantly improved in recent years due to better management.
Vaccination in SLE
The disease and drugs increase susceptibility to various infections in SLE cases. Infections are a major cause of morbidity and mortality SLE. Vaccination against pneumococci, meningococci, influenza, and Hepatitis-B is strongly recommended. Live vaccines such as measles, mumps, rubella, polio, and varicella should not be used in patients on medium to high-dose glucocorticoids and immunosuppressant drugs.
