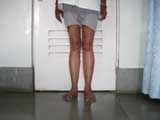
 Valgus Knees |
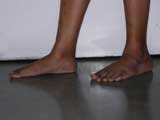 Flat Foot |
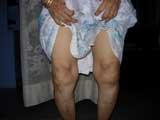 Knee Osteoarthritis |
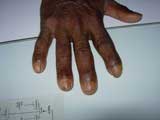 Hand Osteoarthritis |
Osteoarthritis (OA) affects about 4-6% of the adult population and is listed in India's top 5 chronic diseases. It is a common, age-related, chronic, and slowly progressive joint disorder that ultimately leads to joint failure. The most common joints involved in the osteoarthritic process are those which overwork during entire life, viz. knees, neck, low back, and small hand joints at the fingertips. It is a disease of cartilage – a smooth rubbery cushion covering the surfaces of bones of the joint. It contains few cells which secrete a complex matrix made up of proteoglycans and hyaluronic acid. Worn-out matrix components are regularly replaced during life, although cartilage has a very limited ability to repair and adapt. Cartilage breakdown in OA is associated with damage to menisci and other joint components and bone remodeling. It is not a disease of aging because about 45% of people above 100 years do not have any pain due to OA. Half of the elderly patients with knee pain have normal knee X-rays. OA is currently considered a disease caused by a dynamic reaction of the joint to various biomechanical and biochemical factors. It occurs when the degradation of cartilage exceeds repair. The ligaments surrounding the joint become lax, the joint capsule thickens, the joint fluid becomes less viscous, muscles undergo wasting, and become weak. These changes ultimately lead to joint failure - a condition akin to heart failure or kidney failure. Cartilage has no pain sensation. Pain in OA arises from bone and other structures within and around the joint. Crystals and swelling inside the joint are important causes of pain in OA.
Causes
Age (weakness, joint laxity, decreased sensory capacities), female sex (after menopause - especially if the uterus is surgically removed), and being overweight are the main risk factors for the development of OA. There is a direct correlation between obesity and osteoarthritis due to certain chemicals (adipokines) secreted by cells of the fatty tissues. OA is also known to run in some families. Although heredity plays a very small role in OA, the involvement of small hand joints and onset at a younger age are common features in such patients. Certain mechanical factors such as joint hypermobility, previous surgery or injury, repetitive joint use (occupational, e.g., farmers and porters), and joint deformities (congenital or disease-related) also lead to early OA.
Indian habits of sitting cross-legged, squatting, and kneeling probably accelerate the OA process in knees due to mechanical factors. Secondary OA can develop in diseases such as diabetes and leprosy (neuropathic joint – Charcot's). Other congenital, metabolic, and endocrine disorders can also lead to secondary OA. Secondary OA usually involves atypical joints.
Features
Pain in the involved joint, especially after an activity, is the main feature of OA. There may be some associated stiffness. Morning stiffness does not last for more than half an hour, and stiffness after rest (gelling) lasts for just a few minutes. The pain increases in cold and damp weather in some patients.
The pain usually waxes and wanes in the early stages. There may be intermittent inflammatory flares with severe pain and swelling. Night pain and crepitus (creaking in the joint) are some of the later features. It may be difficult walking upstairs or downstairs, standing for a long time, doing household tasks, getting in or out of an autorickshaw or a car, and getting up from sitting when knees are affected. Hand OA leads to difficulty while opening the lid of a container, writing with a pen, holding or lifting a utensil, and operating door handle or latch-keys. Joints become unstable with the progression of the disease, and movements get restricted along with wasting of muscles. Locking and buckling are other mechanical features. Hands become square-shaped in hand OA, whereas gait changes due to hip or knee OA. Knee OA can be complicated with swellings around the joints (e.g., Baker's cyst, anserine bursitis).
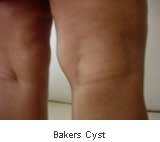 A Baker's cyst can rupture and cause painful swelling of the entire leg. OA of the spine (spondylosis) commonly affects neck and low back regions. Pain on movement, especially after day-long work, is an important feature. Bony overgrowths and changes in disc dimensions can cause pressure on outgoing nerve roots and lead to tingling, numbness, pain, and weakness of hands and legs in the cervical (neck) and lumbar (low back) spondylosis, respectively.
A Baker's cyst can rupture and cause painful swelling of the entire leg. OA of the spine (spondylosis) commonly affects neck and low back regions. Pain on movement, especially after day-long work, is an important feature. Bony overgrowths and changes in disc dimensions can cause pressure on outgoing nerve roots and lead to tingling, numbness, pain, and weakness of hands and legs in the cervical (neck) and lumbar (low back) spondylosis, respectively.
Patterns of OA
OA is probably not a single disease. It can involve a single joint like knee (hip being uncommon in India) or multiple joints. Generalized OA affects more than three joints, usually those of hands. Localized OA manifests as small nodules (Heberden's nodes) around joints near fingertips. OA can be erosive with intermittent painful flares. About 15% of such patients evolve into rheumatoid arthritis.
Investigations
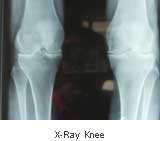
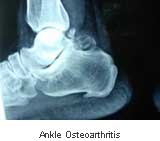 No laboratory tests are required for the diagnosis of OA. The diagnosis can be easily reached from patient history and clinical examination. X-Rays of involved joints can help grade the severity of joint involvement. Medical management can be planned based on the severity of OA. New laboratory tests, including MRI, are being developed as a research tool for the early diagnosis of cartilage degradation. OA disease scores (which measure pain, stiffness, and physical function through a questionnaire) have been developed and help follow the disease progression and response to therapy.
No laboratory tests are required for the diagnosis of OA. The diagnosis can be easily reached from patient history and clinical examination. X-Rays of involved joints can help grade the severity of joint involvement. Medical management can be planned based on the severity of OA. New laboratory tests, including MRI, are being developed as a research tool for the early diagnosis of cartilage degradation. OA disease scores (which measure pain, stiffness, and physical function through a questionnaire) have been developed and help follow the disease progression and response to therapy.
Management
Non-drug therapy is vital in OA management. All patients must learn more about their disease and try to live with it as there is no cure for this chronic condition. Lifestyle changes (pacing of activities-intermittent rest), avoidance of squatting, kneeling, or sitting cross-legged, exercise (both aerobic and joint strengthening – under the guidance of a physiotherapist), and weight reduction are essential for control of OA pain. It is estimated that 10% weight loss reduces OA pain by about 50%. Exercise reduces pain and improves joint function. Regular Yoga practice also helps in various ways. Some patients may require assistive devices such as a stick (hold in opposite hand) and walkers (if both knees are affected) for unloading. The knee cap stabilizes the knee and corrects mild deformities. Moreover, appropriate footwear should be used after assessment from an occupational therapist. Some patients benefit from heat, ice packs, and local ointments/liniments. Capsaicin has shown some benefit on a regular local application for over two months.
Pain management can be done with paracetamol (up to 4 grams per day). A combination of tramadol with paracetamol gives better pain relief. Nonsteroidal anti-inflammatory drugs (ibuprofen, piroxicam, diclofenac, etc.) should be used during inflammatory flares for a short period under medical supervision. These drugs should be used in the lowest possible dose to avoid potential adverse effects. Patients may adjust the doses themselves according to the need for adequate pain control. Severe pain nonresponsive to oral drugs responds well to steroid injection in joint. This simple, safe and effective procedure relieves pain for 3-4 or more months, especially if extra joint fluid is also removed simultaneously. Diacerine, glucosamine, and chondroitin are disease-modifying drugs of doubtful efficacy available for treatment in early OA. They should not be continued for more than 3-6 months if there is no apparent benefit.
Knowledge about the disease, regular exercise, a healthy diet, and adequate sleep are essential elements of OA management. In addition, one must learn to protect joints by avoiding overuse while remaining active. A positive approach towards life and support from family and friends help in coping with this disease.
Surgery
Joint replacement surgery is usually undertaken as a last resort and is expensive. Surgery should be considered in all patients with inadequate pain control and functional improvement despite rigorous drug- and non-drug- therapy. A successful surgery offers excellent pain relief and should not be delayed whenever indicated.
