Rheumatoid arthritis (RA) affects about 0.92% of the adult population in India. It a systemic autoimmune disease which leads to swelling (inflammation) of various joints. The swelling destroys joints from within and causes permanent deformities. Effective treatments are now available for this common disease. Early diagnosis and aggressive therapy can usually prevent permanent disability. Unfortunately, this does not happen in many cases. There are about 20-40 new cases per Lac population each year, and the disease occurs more frequently in females. The onset can be after delivery, although the disease remains silent during pregnancy. Stress and environmental triggers can precipitate the onset of the disease. About 5% of first-degree relatives are at risk of developing RA. Cigarette smoking, coffee, and oral contraceptive pills appear to increase the risk of its development. Early diagnosis is the key to prevent deformities with appropriate management. Delay in diagnosis is the leading cause of functional disability and reduced quality of life.
Symptoms
Swelling of three or more joints, involvement of small joints of hands and wrists, symmetry of joint involvement, and morning stiffness lasting for over an hour are the main features of the disease according to earlier criteria laid down by the American College of Rheumatology. However, these have been modified to add more weightage to the involvement of small joints of hands and values of some blood tests such as Rheumatoid Factor (RF- RA Factor is incorrect) and Anti-cyclic Citrullinated Peptide Antibodies (ACPA).
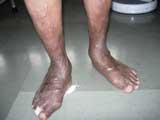
The disease usually starts insidiously with the involvement of few joints and affects more number of joints later on. RA can sometimes begin and remain confined to a single joint, such as the knee joint. Some generalized features such as feverishness, weakness, fatigue, malaise, loss of appetite (anorexia), and hair loss may also accompany. Anxiety, depression, helplessness, and loss of confidence are usually observed in chronic cases. The joints are progressively damaged in untreated or inadequately treated patients and develop various deformities such as deviated fingers, swan neck fingers, finger subluxation, hammertoes, flat feet, and fixed contractures of large joints. Many diseases can mimic RA. Therefore, an expert rheumatologist is needed to establish the diagnosis and plan customized therapy for every patient.
Involvement of other systems
Rheumatoid Vasculitis: Uncontrolled RA is now recognized to reduce lifespan by about seven years due to the involvement of blood vessels. RA can involve various systems in our body. Male patients and those with positive rheumatoid factors are more likely to develop extra-articular features. Some of these problems can also develop due to intercurrent infections and cancers. Thorough investigations are, therefore, essential in such cases.
Common problems are given in the following table:
| 1 | Bones | Osteoporosis (Weak bones with increased fracture risk). |
| 2 | Muscles | Wasting and weakness. |
| 3 | Eyes | Dryness, pain and redness, ulceration and perforation. |
| 4 | Lungs | Pleural effusion (fluid around lungs), Interstitial pneumonia and fibrosis. |
| 5 | Mucosa | Dry mouth, vaginal dryness. |
| 6 | Heart | Effusion (fluid around heart), swelling of heart (myocarditis). |
| 7 | Nodules | Painless nodules on back of forearm and other areas. Can occur in lungs and other organs too. |
| 8 | Blood | Anemia, reduced white cells and platelets. |
| 9 | Blood Vessels | Arteriosclerosis – thickening and stiffness of vessels. Higher risk of heart attack and strokes. More severe heart disease. Early death. |
| 10 | Vasculitis | Swelling of blood vessels. Nonhealing skin ulcers and infections. Neuropathy. |
| 11 | Nerves | Neuropathy |
| 12 | Kidneys | Glomerulonephritis and interstitial nephritis. |
| 13 | Psychological | Anxiety, depression. |
| 14 | Infections | High risk. |
| 15 | Cancers | Lymphoproliferative – high risk. |
| 16 | Others | Hoarse voice, ringing in ears, amyloid. |
| 17 | Drugs | Many systemic adverse events. |
Investigations
Erythrocyte sedimentation rate (ESR) and C-reactive proteins (CRP) are the blood tests that indicate inflammation. RF and ACPA indicate immune dysfunction, and higher levels increase the possibility of RA. However, RF positivity does not automatically mean RA as 3% of the average population (especially aged) is RF positive. RF positivity is seen in many other conditions such as diabetes, liver disease, cancer, TB, and AIDS. Diagnosis of RA is clinical, and the presence of joint swelling (synovitis) is essential for diagnosis. Other blood tests are required to assess systemic involvement (liver, kidneys, etc.) and monitor adverse drug events. X-rays of joints may indicate destruction and bone loss. Ultrasound and magnetic resonance examination of joints can detect joint involvement at a very early stage.
Early RA
All cases of swelling of more than one joint must be seen by a rheumatologist, preferably within six weeks, as joint damage can be prevented by aggressive therapy at this stage. Female sex, a higher number of involved joints, RF/ACPA positivity, high ESR/CRP levels indicate a diagnosis of RA and predict severe disease. RA of less than two-year duration is known as early disease. In contrast, a duration of fewer than three months indicates a very early disease.
Assessment
Disease assessment in RA is extremely important for knowing the severity and activity of the disease. Such assessment also helps in planning and monitoring therapy. Various disease activity scores such as DAS-28 (28 joints examined for swelling and tenderness) and CDAI (a clinical disease activity score that does not require any blood examinations) have now been validated for the evaluation of RA. Pain, fatigue, quality of life, and other assessments are needed to be carried out in clinical research. A simple health assessment questionnaire has also been devised for patients with RA. The American College of Rheumatology and European League against Rheumatism have developed criteria for disease remission, which indicate treatment efficacy and help modifications in therapy.
Management
Significant progress has been made recently in the drug management of this disabling disease. Many drugs, if used appropriately, can slow down the disease progression. Although there is no permanent cure, the current research aims to halting or reversing joint damage and achieving complete remission. The therapy goals are to relieve pain and stiffness, control the disease, and avert possible disease complications. Pain and inflammation are managed with paracetamol, nonsteroidal anti-inflammatory drugs (ibuprofen, piroxicam, indomethacin, etc.), and glucocorticoids. These drugs are used as "bridge" therapy until disease-modifying antirheumatic drugs (DMARDs) take over disease control. DMARDs usually require 2-6 months for maximum benefit. Painkillers and glucocorticoids (steroids) can then be reduced or entirely stopped according to patient response. DMARDs commonly used are hydroxychloroquine (200-400 mg once daily-preferably at night), sulfasalazine (2 to 4 grams a day in divided doses), methotrexate (10-25 mg oral tablet or subcutaneous injection once a week), and leflunomide (10-20 mg once daily).
All DMARDs can cause adverse effects in a few patients and need to be monitored by a rheumatologist. New biologic agents (etanercept, infliximab, adalimumab, abatacept, rituximab, etc.) have shown dramatic effects in methotrexate nonresponsive cases. Though effective, they are expensive and unaffordable for most Indian patients. Many new drugs are in the pipeline, and coming years will see a revolution in RA management. Drug compliance as per rheumatological advice is crucial. It is observed that 50% of uncontrolled patients are non-compliant. Lifetime use of DMARDs is recommended at present. However, their dosages can be reduced after achieving adequate control of disease activity.
Lifestyle
Healthy living and positive thinking are essential for all patients of RA. One must understand the disease and learn to live with it. Active lifestyle, regular exercise(aerobic – walking, swimming, Yoga), weight control, adequate rest, avoidance of smoking and alcohol, and nutritious food (proteins, calories, and calcium) habits are self-care essentials. The role of a particular diet has no scientific proof as yet. Physiotherapy (range of motion and strengthening exercises)-under the guidance of a physiotherapist- is used to maintain joint shape and function. Splints, gadgets, and other appliances compensate for joint deformities. Application of heat, cold, or ointment can relieve pain in some cases. Overexertion should be avoided. Adequate rest is essential during disease flares. RA is a chronic disease and can lead to anxiety and depression. Support groups can be of great help in these situations.
Surgery
RA affects many joints at the same time. Drug treatment, therefore, is the mainstay of treatment. Joint replacement or other operations are indicated in deformed joints with functional impairment. Knee or hip replacement, ankle or wrist fusions are some of the surgeries required for deformed joints. Surgery is usually expensive. It is not the final answer, and drugs must be continued even after a successful surgery.